Important Safety Information
MITRACLIP
INDICATION FOR USE • The MitraClipTM G4 System is indicated for the percutaneous reduction of significant symptomatic mitral regurgitation (MR ≥ 3+) due to primary abnormality of the mitral apparatus [degenerative MR] in patients who have been determined to be at prohibitive risk for mitral valve surgery by a heart team, which includes a cardiac surgeon experienced in mitral valve surgery and a cardiologist experienced in mitral valve disease, and in whom existing comorbidities would not preclude the expected benefit from reduction of the mitral regurgitation. • The MitraClipTM G4 System, when used with maximally tolerated guideline-directed medical therapy (GDMT), is indicated for the treatment of symptomatic, moderateto-severe or severe secondary (or functional) mitral regurgitation (MR; MR ≥ Grade III per American Society of Echocardiography criteria) in patients with a left ventricular ejection fraction (LVEF) ≥ 20% and ≤ 50%, and a left ventricular end systolic dimension (LVESD) ≤ 70 mm whose symptoms and MR severity persist despite maximally tolerated GDMT as determined by a multidisciplinary heart team experienced in the evaluation and treatment of heart failure and mitral valve disease. CONTRAINDICATIONS The MitraClipTM G4 System is contraindicated in patients with the following conditions: • Patients who cannot tolerate, including allergy or hypersensitivity to, procedural anticoagulation or post procedural anti-platelet regimen • Patients with known hypersensitivity to clip components (nickel / titanium, cobalt, chromium, polyester), or with contrast sensitivity • Active endocarditis of the mitral valve • Rheumatic mitral valve disease • Evidence of intracardiac, inferior vena cava (IVC) or femoral venous thrombus WARNINGS • DO NOT use MitraClipTM outside of the labeled indication. • The MitraClipTM G4 Implant should be implanted with sterile techniques using fluoroscopy and echocardiography (e.g. transesophageal [TEE] and transthoracic [TTE]) in a facility with on-site cardiac surgery and immediate access to a cardiac operating room. • Read all instructions carefully. Use universal precautions for biohazards and sharps while handling the MitraClipTM G4 System to avoid user injury. Failure to follow these instructions, warnings and precautions may lead to device damage, user injury or patient injury including: n MitraClipTM G4 Implant erosion, migration or malposition n Failure to deliver MitraClipTM G4 Implant to the intended site n Difficulty or failure to retrieve MitraClipTM G4 system components • Use caution when treating patients with hemodynamic instability requiring inotropic support or mechanical heart assistance due to the increased risk of mortality in this patient population. The safety and effectiveness of MitraClipTM in these patients has not been evaluated. • Patients with a rotated heart due to prior cardiac surgery in whom the System is used may have a potential risk of experiencing adverse events such as atrial perforation, cardiac tamponade, tissue damage, and embolism which may be avoided with preoperative evaluation and proper device usage. • For the Steerable Guide Catheter and Delivery Catheter only: n The Guide Catheter: the distal 65 cm of the Steerable Guide Catheter with the exception of the distal soft tip, is coated with a hydrophilic coating. n The Delivery Catheter: coated with a hydrophilic coating for a length of approximately 131 cm. n Failure to prepare the device as stated in these instructions and failure to handle the device with care could lead to additional intervention or serious adverse event. • The Clip Delivery System is provided sterile and designed for single use only. Cleaning, re-sterilization and / or reuse may result in infections, malfunction of the device and other serious injury or death. • Note the product “Use by” date specified on the package. • Inspect all product prior to use. Do not use if the package is open or damaged, or if product is damaged. PRECAUTIONS • Prohibitive Risk Primary (or degenerative) Mitral Regurgitation n Prohibitive risk is determined by the clinical judgment of a heart team, including a cardiac surgeon experienced in mitral valve surgery and a cardiologist experienced in mitral valve disease, due to the presence of one or more of the following documented surgical risk factors: ◆ 30-day STS predicted operative mortality risk score of 4 ≥8% for patients deemed likely to undergo mitral valve replacement or 4 ≥6% for patients deemed likely to undergo mitral valve repair n Porcelain aorta or extensively calcified ascending aorta. n Frailty (assessed by in-person cardiac surgeon consultation) n Hostile chest n Severe liver disease / cirrhosis (MELD Score > 12) n Severe pulmonary hypertension (systolic pulmonary artery pressure > 2/3 systemic pressure) n Unusual extenuating circumstance, such as right ventricular dysfunction with severe tricuspid regurgitation, chemotherapy for malignancy, major bleeding diathesis, immobility, AIDS, severe dementia, high risk of aspiration, internal mammary artery (IMA) at high risk of injury, etc. n Evaluable data regarding safety or effectiveness is not available for prohibitive risk Primary patients with an LVEF < 20% or an LVESD > 60 mm. MitraClipTM should be used only when criteria for clip suitability for Primary have been met. n The heart team should include a cardiac surgeon experienced in mitral valve surgery and a cardiologist experienced in mitral valve disease and may also include appropriate physicians to assess the adequacy of heart failure treatment and valvular anatomy. • Secondary Mitral Regurgitation n Evaluable data regarding safety or effectiveness is not available for secondary MR patients with an LVEF < 20% or an LVESD > 70 mm. n The multidisciplinary heart team should be experienced in the evaluation and treatment of heart failure and mitral valve disease and determine that symptoms and MR severity persist despite maximally tolerated GDMT. POTENTIAL COMPLICATIONS AND ADVERSE EVENTS The following ANTICIPATED EVENTS have been identified as possible complications of the MitraClipTM G4 procedure. • Allergic reactions or hypersensitivity to latex, contrast agent, anaesthesia, device materials (nickel / titanium, cobalt, chromium, polyester), and drug reactions to anticoagulation, or antiplatelet drugs • Vascular access complications which may require transfusion or vessel repair including: n wound dehiscence n catheter site reactions n Bleeding (including ecchymosis, oozing, hematoma, hemorrhage, retroperitoneal hemorrhage) n Arteriovenous fistula, pseudoaneurysm, aneurysm, dissection, perforation / rupture, vascular occlusion n Emboli (air thrombotic material, implant, device component) n Peripheral Nerve Injury • Lymphatic complications • Pericardial complications which may require additional intervention, including: n Pericardial effusion n Cardiac tamponade n Pericarditis • Cardiac complications which may require additional interventions or emergency cardiac surgery, including: n Cardiac perforation n Atrial septal defect • Mitral valve complications, which may complicate or prevent later surgical repair, including: n Chordal entanglement / rupture n Single Leaflet Device Attachment (SLDA) n Thrombosis n Dislodgement of previously implanted devices n Tissue damage n Mitral valve stenosis n Persistent or residual mitral regurgitation n Endocarditis • Cardiac arrhythmias (including conduction disorders, atrial arrhythmias, ventricular arrhythmias) • Cardiac ischemic conditions (including myocardial infarction, myocardial ischemia, and unstable / stable angina) • Venous thromboembolism (including deep vein thrombosis, pulmonary embolism, post procedure pulmonary embolism) • Stroke / Cerebrovascular accident (CVA) and Transient Ischemic Attack (TIA) • System organ failure: n Cardio-respiratory arrest n Worsening heart failure n Pulmonary congestion n Respiratory dysfunction / failure / atelectasis n Renal insufficiency or failure n Shock (including cardiogenic and anaphylactic) • Blood cell disorders (including coagulopathy, hemolysis, and Heparin Induced Thrombocytopenia (HIT)) • Hypotension / hypertension • Infection including: n Urinary Tract Infection (UTI) n Pneumonia n Septicemia • Nausea / vomiting • Chest pain • Dyspnea • Edema • Fever or hyperthermia • Pain • Death • Fluoroscopy, Transesophageal echocardiogram (TEE) and Transthoracic echocardiogram (TTE) -related complications: n Skin injury or tissue changes due to exposure to ionizing radiation n Esophageal irritation n Esophageal perforation n Gastrointestinal bleeding.
Caution: This product is intended for use by or under the direction of a physician. Prior to use, reference the Instructions for Use provided inside the product carton (when available) or at eifu.abbottvascular.com or at medical.abbott/manuals for more detailed information on Indications, Contraindications, Warnings, Precautions and Adverse Events. TM Indicates a trademark of the Abbott Group of Companies. www.Cardiovascular.Abbott
PICCOLO
https://www.structuralheartsolutions.com/fileadmin/us/piccolo-ISI.pdf
INDICATIONS AND USAGE The AMPLATZER Piccolo™ Occluder is a percutaneous, transcatheter occlusion device intended for the nonsurgical closure of a patent ductus arteriosus (PDA). CONTRAINDICATIONS • Weight < 700 grams at time of the procedure • Age < 3 days at time of procedure • Coarctation of the aorta • Left pulmonary artery stenosis • Cardiac output that is dependent on right to left shunt through the PDA due to pulmonary hypertension • Intracardiac thrombus that may interfere with the implant procedure • Active infection requiring treatment at the time of implant • Patients with a PDA length smaller than 3 mm • Patients with a PDA diameter that is greater than 4 mm at the narrowest portion WARNINGS • This device was sterilized with ethylene oxide and is for single use only. Do not reuse or re-sterilize this device. Attempts to resterilize this device can cause a malfunction, insufficient sterilization, or harm to the patient. • Do not use the device if the sterile package is open or damaged. • Use on or before the last day of the expiration month that is printed on the product packaging label. • Patients who are allergic to nickel can have an allergic reaction to this device. • Prepare for situations that require the removal of this device. Preparation includes access to a transcatheter snare kit and an on-site surgeon. • Accurate measurements of the ductus are crucial for correct occluder size selection. • Do not release the occluder from the delivery wire if either a retention disc protrudes into the pulmonary artery or aorta; or if the position of the occluder is not stable. • Remove embolized devices. Do not remove an embolized occluder through intracardiac structures unless the occluder is fully recaptured inside a catheter. PRECAUTIONS • This device should be used only by physicians who are trained in standard transcatheter techniques. Determine which patients are candidates for procedures that use this device. • The physician should exercise clinical judgment in situations that involve the use of anticoagulants and antiplatelet drugs before, during, and/or after the use of this device. • Patients should have an activated clotting time (ACT) of greater than 200 sec prior to device placement, unless the patient has a significant risk for bleeding and is unable to be anti-coagulated. • The device may be delivered via an anterograde (venous) or a retrograde (arterial) approach. However, in small infants (≤2 kg), the device should be delivered using the anterograde (venous) approach since small infants are at an increased risk for arterial injury. • The AMPLATZER Piccolo™ Occluder contains nickel-titanium alloy, which is generally considered safe. However, in vitro testing has demonstrated that nickel is released from this device for a minimum of 60 days following implant. Patients who are allergic to nickel may have an allergic reaction to this device, especially those with a history of metal allergies. Certain allergic reactions can be serious; patients should seek immediate medical attention if there is suspicion of an allergic reaction. Symptoms may include difficulty in breathing or swelling of the face or throat. While data are currently limited, it is possible that some patients may develop an allergy to nickel if this device is implanted. • Use in specific populations n Pregnancy — Minimize radiation exposure to the fetus and the mother. n Nursing mothers — There has been no quantitative assessment for the presence of leachables in breast milk. • Store in a dry place. • Do not use contrast power injection with delivery catheter. POTENTIAL ADVERSE EVENTS Potential adverse events that may occur during or after a procedure placing this device include, but are not limited to: • Air embolus • Allergic dye reaction • Allergic drug reaction • Anesthesia reactions • Apnea • Arrhythmia • Bacterial endocarditis • Bleeding • Cardiac perforation • Cardiac tamponade • Chest pain • Device embolization • Device erosion • Death • Fever • Headache/migraine • Hemolysis • Hematoma • Hypertension • Hypotension • Infection • Myocardial infarction • Palpitations • Partial obstruction of aorta • Partial obstruction of pulmonary artery • Pericardial effusion • Pericarditis • Peripheral embolism • Pleural effusion • Pulmonary embolism • Re-intervention for device removal • Respiratory distress • Stroke • Thrombus • Transient ischemic attack • Valvular regurgitation • Vascular access site injury • Vascular occlusion • Vessel perforation.
CAUTION: This product is intended for use by or under the direction of a physician. Prior to use, reference the Instructions for Use, inside the product carton (when available) or at eifu.abbottvascular.com or at medical.abbott/manuals for more detailed information on Indications, Contraindications, Warnings, Precautions and Adverse Events. ™ Indicates a trademark of the Abbott group of companies. ‡ Indicates a third-party trademark, which is property of its respective owner.
MASTERS
https://www.vascular.abbott/content/dam/bss/divisionalsites/av/products/valve-sizer-isi.pdf
RX ONLY
INDICATIONS FOR USE
The SJM™ Masters Series Mechanical Heart Valve is intended for use as a replacement valve in patients with a diseased, damaged, or malfunctioning mitral or aortic heart valve. This device may also be used to replace a previously implanted mitral or aortic prosthetic heart valve. The sizer model 905-15 is indicated to confirm size selection of the 15AHPJ-505 and 15MHPJ-505 valves.
CONTRAINDICATIONS
The SJM™ Masters Series Mechanical Heart Valve is contraindicated for individuals unable to tolerate anticoagulation therapy. The sizer model 905-15 is contraindicated for use with any devices other than the 15 AHPJ-505 and 15MHPJ-505 valves. Any sizer sterilization method other than steam is contraindicated.
WARNINGS
Valve
For single use only. Attempts to reuse the valve may result in valve malfunction, inadequate sterilization, or patient harm. Use only St. Jude Medical™ mechanical heart valve sizers.
Do not use if: The valve has been dropped, damaged, or mishandled in any way.
The expiration date has elapsed.
The tamper-evident container seal or inner/ outer tray seals are damaged, broken, or missing.
Remove any residual tissue that may impair valve size selection, correct seating of the valve, rotation of the valve, or leaflet motion.
Proper valve size selection is crucial. Do not oversize the valve. If the native annulus measurement falls between two SJM™ Masters Series Mechanical Heart Valve sizes, use the smaller prosthetic valve size.
The outer tray is not sterile, and should not be placed in the sterile field.
To minimize direct handling of the valve during implantation, do not remove the holder/rotator until the valve has been seated in the annulus.
Do not use hard or rigid instruments to test leaflet mobility, as this may result in structural damage to the valve or thromboembolic complications. Use a St. Jude Medical™ leaflet tester to gently test valve leaflet mobility.
Place sutures in the outer half of the valve sewing cuff.
Never apply force to the valve leaflets. Force may cause structural damage to the valve.
Use only SJM™ Valve Holder/Rotators to perform valve rotation. Use of other instruments could result in structural damage. The valve holder/rotator is intended for single use only and should be discarded after surgery.
The two retention sutures on the valve holder/ rotator must be cut and removed before the valve can be rotated.
Do not pass catheters or other instruments through St. Jude Medical™ mechanical heart valves. This could result in scratched or damaged valve components, leaflet fracture, or dislodgment.
Cut suture ends short, especially in the vicinity of the pivot guards, to prevent leaflet impingement
PRECAUTIONS
Valve
Do not touch the prosthetic valve unnecessarily, even with gloved hands. This may cause scratches or surface imperfections that may lead to thrombus formation.
Be careful not to cut or tear the valve sewing cuff when removing the identification tag and the holder/rotator from the valve.
Before placing sutures in the valve sewing cuff, verify that the valve is mounted correctly on the valve holder/rotator.
To avoid structural damage, the valve must be rotated in the fully open position.
To minimize rotational torque, verify that the valve holder/rotator is properly seated in the valve, and that the valve holder handle is perpendicular to the valve.
Remove any loose suture or thread, which may be a source of thrombus or thromboembolism.
Implantation of a prosthetic valve too large for the annulus may result in increased risk of damage to the conductive system, obstruction of the left ventricular outflow tract, impairment of valve mobility, damage to the left circumflex artery, and damage to surrounding tissues or cardiac structures including obstruction and/or distortion of adjacent cardiac structures.
NOTE: PROSPECTIVE DATA TO SUPPORT SAFETY AND EFFECTIVENESS OF THE 15-mm HP VALVE IMPLANTED IN THE AORTIC POSITION ARE NOT CURRENTLY AVAILABLE.
Sizer
Instruments must be cleaned and sterilized prior to use.
Do not use cracked, deformed, discolored/rusted, or damaged instruments.
Improper cleaning may result in an immunological or toxic reaction.
Instrument sterilization temperature must not exceed 280°F (138°C).
Do not bend flexible instrument handles beyond a 90° angle.
Instruments must be sterilized in a tray or container that is permeable to steam.
Do not expose instruments to cleaning or rinse agents that are not compatible with polysulfone or polyphenylsulfone.
POTENTIAL ADVERSE EVENTS
Complications associated with replacement mechanical heart valves include, but are not limited to, hemolysis, infections, thrombus, or thromboembolism, valve dehiscence, unacceptable hemodynamic performance, hemorrhagic complications secondary to anticoagulation therapy, heart block requiring pacemaker implant, prosthetic failure, adjacent cardiac structure interference, heart failure, stroke, myocardial infarction, or death. Any of these complications may require reoperation or explantation of the device.
Related articles
-
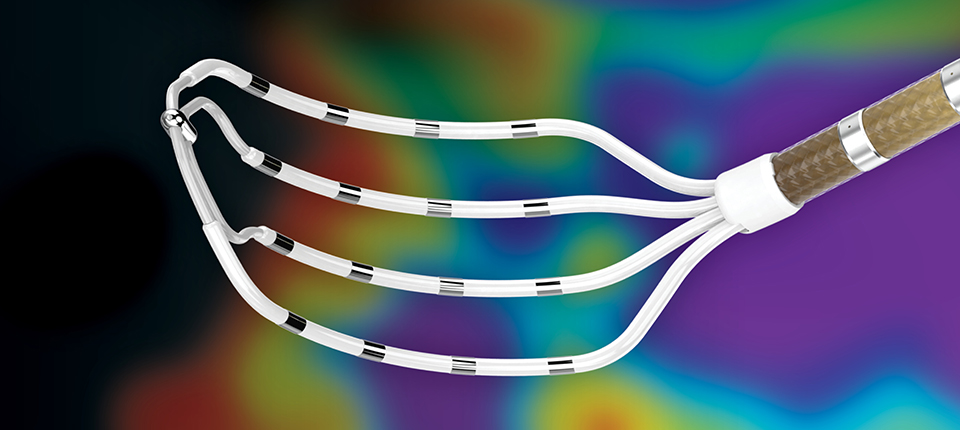
Cardiac Mapping: Changing the Game With Advisor HD Grid
With a vibrant mix of reds, purples and greens, Abbott's cardiac mapping tool is like HDTV for the heart — and it's a sight to behold.
-
"Just Like Meeting in the Office": This is Telehealth.
For people living with chronic conditions during COVID-19, telehealth can bridge to their doctors.