Important Safety Information
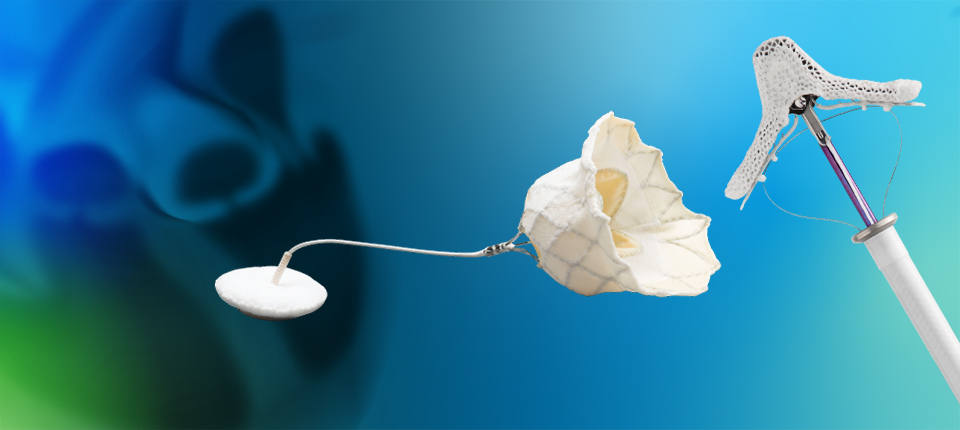
MITRACLIP CLIP DELIVERY SYSTEMS
INDICATION FOR USE
- The MitraClip™ NTR/XTR System is indicated for the percutaneous reduction of significant symptomatic mitral regurgitation (MR ≥ 3+) due to primary abnormality of the mitral apparatus [degenerative MR] in patients who have been determined to be at prohibitive risk for mitral valve surgery by a heart team, which includes a cardiac surgeon experienced in mitral valve surgery and a cardiologist experienced in mitral valve disease, and in whom existing comorbidities would not preclude the expected benefit from reduction of the mitral regurgitation.
- The MitraClip™ NTR/XTR System, when used with maximally tolerated guideline-directed medical therapy (GDMT), is indicated for the treatment of symptomatic, moderate-to-severe or severe secondary (or functional) mitral regurgitation (MR; MR ≥ Grade III per American Society of Echocardiography criteria) in patients with a left ventricular ejection fraction (LVEF) ≥ 20% and ≤ 50%, and a left ventricular end systolic dimension (LVESD) ≤ 70 mm whose symptoms and MR severity persist despite maximally tolerated GDMT as determined by a multidisciplinary heart team experienced in the evaluation and treatment of heart failure and mitral valve disease.
CONTRAINDICATIONS
The MitraClip™ NTR/XTR System is contraindicated in patients with the following conditions:
- Patients who cannot tolerate procedural anticoagulation or post procedural anti-platelet regimen
- Active endocarditis of the mitral valve
- Rheumatic mitral valve disease
- Evidence of intracardiac, inferior vena cava (IVC) or femoral venous thrombus
WARNINGS
- DO NOT use MitraClip™ outside of the labeled indication.
- The MitraClip™ Implant should be implanted with sterile techniques using fluoroscopy and echocardiography (e.g., transesophageal [TEE] and transthoracic [TTE]) in a facility with on-site cardiac surgery and immediate access to a cardiac operating room.
- Read all instructions carefully. Failure to follow these instructions, warnings and precautions may lead to device damage, user injury or patient injury. Use universal precautions for biohazards and sharps while handling the MitraClip™ System to avoid user injury.
- Use of the MitraClip™ should be restricted to those physicians trained to perform invasive endovascular and transseptal procedures and those trained in the proper use of the system.
- The Clip Delivery System is provided sterile and designed for single use only. Cleaning, re-sterilization and / or reuse may result in infections, malfunction of the device or other serious injury or death.
- Use caution when treating patients with hemodynamic instability requiring inotropic support or mechanical heart assistance due to the increased risk of mortality in this patient population. The safety and effectiveness of MitraClip™ in these patients has not been evaluated.
PRECAUTIONS
- Note the product “Use by” date specified on the package.
- Inspect all product prior to use. Do not use if the package is open or damaged, or if product is damaged.
- Prohibitive Risk Primary (or degenerative) Mitral Regurgitation
- Prohibitive risk is determined by the clinical judgment of a heart team, including a cardiac surgeon experienced in mitral valve surgery and a cardiologist experienced in mitral valve disease, due to the presence of one or more of the following documented surgical risk factors:
- 30-day STS predicted operative mortality risk score of
- ≥8% for patients deemed likely to undergo mitral valve replacement or
- ≥6% for patients deemed likely to undergo mitral valve repair
- Porcelain aorta or extensively calcified ascending aorta.
- Frailty (assessed by in-person cardiac surgeon consultation).
- Hostile chest
- Severe liver disease / cirrhosis (MELD Score > 12)
- Severe pulmonary hypertension (systolic pulmonary artery pressure > 2/3 systemic pressure)
- Unusual extenuating circumstance, such as right ventricular dysfunction with severe tricuspid regurgitation, chemotherapy for malignancy, major bleeding diathesis, immobility, AIDS, severe dementia, high risk of aspiration, internal mammary artery(IMA) at high risk of injury, etc.
- Evaluable data regarding safety or effectiveness is not available for prohibitive risk DMR patients with an LVEF < 20% or an LVESD > 60 mm. MitraClip® should be used only when criteria for clip suitability for DMR have been met.
- The heart team should include a cardiac surgeon experienced in mitral valve surgery and a cardiologist experienced in mitral valve disease and may also include appropriate physicians to assess the adequacy of heart failure treatment and valvular anatomy.
- Secondary Mitral Regurgitation
- Evaluable data regarding safety or effectiveness is not available for secondary MR patients with an LVEF < 20% or an LVESD > 70 mm.
- The multidisciplinary heart team should be experienced in the evaluation and treatment of heart failure and mitral valve disease and determine that symptoms and MR severity persist despite maximally tolerated GDMT.
POTENTIAL COMPLICATIONS AND ADVERSE EVENTS
The following ANTICIPATED EVENTS have been identified as possible complications of the MitraClipTM procedure.
Death; Allergic reaction (anesthetic, contrast, Heparin, nickel alloy, latex); Aneurysm or pseudo-aneurysm; Arrhythmias; Atrial fibrillation; Atrial septal defect requiring intervention; Arterio-venous fistula; Bleeding;
Cardiac arrest; Cardiac perforation; Cardiac tamponade / Pericardial Effusion; Chordal entanglement / rupture; Coagulopathy; Conversion to standard valve surgery; Deep venous thrombus (DVT); Dislodgement of previously implanted devices; Dizziness; Drug reaction to anti-platelet / anticoagulation agents / contrast
media; Dyskinesia; Dyspnea; Edema; Emboli (air, thrombus, MitraClipTM Implant); Emergency cardiac surgery; Endocarditis; Esophageal irritation; Esophageal perforation or stricture; Failure to deliver MitraClipTM to the intended site; Failure to retrieve MitraClipTM System components; Fever or hyperthermia; Gastrointestinal bleeding or infarct; Hematoma; Hemolysis; Hemorrhage requiring transfusion; Hypotension / hypertension; Infection; Injury to mitral valve complicating or preventing later surgical repair; Lymphatic complications; Mesenteric ischemia; MitraClipTM Implant erosion, migration or malposition; MitraClipTM Implant thrombosis; MitraClipTM System component(s) embolization; Mitral stenosis; Mitral valve injury; Multi-system organ failure; Myocardial infarction; Nausea / vomiting; Pain; Peripheral ischemia; Prolonged angina; Prolonged ventilation; Pulmonary congestion; Pulmonary thrombo-embolism; Renal insufficiency or failure; Respiratory failure / atelectasis / pneumonia; Septicemia; Shock, Anaphylactic or Cardiogenic; Single leaflet device attachment (SLDA); Skin injury or tissue changes due to exposure to ionizing radiation; Stroke or transient ischemic attack (TIA); Urinary tract infection; Vascular trauma, dissection or occlusion; Vessel spasm; Vessel perforation or laceration; Worsening heart failure; Worsening mitral regurgitation; Wound dehiscence