Important Safety Information
AVEIR LEADLESS PACEMAKER SYSTEM
Rx only
Brief Summary: Prior to using these devices, please review the Instructions for Use for a complete listing of indications, contraindications, warnings, precautions, potential adverse events and directions for use.
Indications: The Aveir™ Leadless Pacemaker system is indicated for management of one or more of the following permanent conditions: Syncope, Pre-syncope, Fatigue, Disorientation. Rate-modulated pacing is indicated for patients with chronotropic incompetence, and for those who would benefit from increased stimulation rates concurrent with physical activity. Dual-chamber pacing is indicated for patients exhibiting: Sick sinus syndrome, Chronic, symptomatic second- and third-degree AV block, Recurrent Adams-Stokes syndrome, Symptomatic bilateral bundle-branch block when tachyarrhythmia and other causes have been ruled out. Atrial pacing is indicated for patients with: Sinus node dysfunction and normal AV and intraventricular conduction systems. Ventricular pacing is indicated for patients with: Significant bradycardia and normal sinus rhythm with only rare episodes of AV block or sinus arrest, Chronic atrial fibrillation, Severe physical disability.
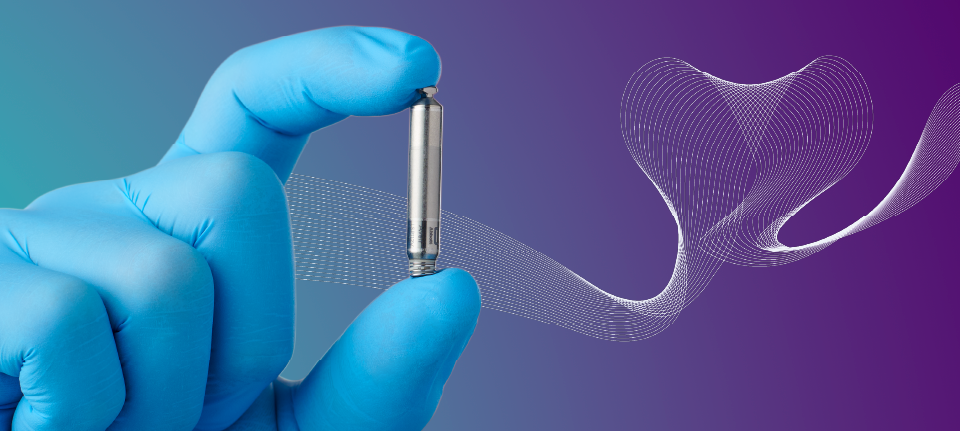
Intended Use: The Aveir™ Leadless Pacemaker (LP) is designed to provide bradycardia pacing as a pulse generator with built-in battery and electrodes for implantation in the right ventricle and/or right atrium. The LP is intended to provide sensing of intrinsic cardiac signals and delivery of cardiac pacing therapy within the implanted chamber for the target treatment group. The LP is also intended to operate optionally with another co-implanted LP to provide dual-chamber pacing therapy.
The Aveir™ Delivery Catheter is intended to be used in the peripheral vasculature and the cardiovascular system to deliver and manipulate an LP. Delivery and manipulation includes implanting an LP within the target chamber of the heart.
Contraindications: Use of the Aveir™ Leadless Pacemaker is contraindicated in these cases:
- Use of any pacemaker is contraindicated in patients with a co-implanted ICD because high-voltage shocks could damage the pacemaker and the pacemaker could reduce shock effectiveness.
- Single-chamber ventricular demand pacing is relatively contraindicated in patients who have demonstrated pacemaker syndrome, have retrograde VA conduction, or suffer a drop in arterial blood pressure with the onset of ventricular pacing.
- Programming of rate-responsive pacing is contraindicated in patients with intolerance of high sensor driven rates.
- Use is contraindicated in patients with an implanted vena cava filter or mechanical tricuspid valve because of interference between these devices and the delivery system during implantation.
- Persons with known history of allergies to any of the components of this device may suffer an allergic reaction to this device. Prior to use on the patient, the patient should be counseled on the materials (listed in the Product Materials section of the IFU) contained in the device and a thorough history of allergies must be discussed.
Adverse Events: Potential complications associated with the use of the Aveir™ Leadless Pacemaker system are the same as with the use of single or dual chamber pacemakers with active fixation pacing leads including, but not limited to: Cardiac perforation, Cardiac tamponade, Pericardial effusion, Pericarditis, Valve damage and/or regurgitation, Heart failure, Pneumothorax/hemothorax, Cardiac arrhythmias, Diaphragmatic/phrenic nerve stimulation / extra-cardiac stimulation, Palpitations, Hypotension, Syncope, Cerebrovascular accident, Infection, Hypersensitivity reaction to device materials, contrast media, medications, or direct toxic effect of contrast media on kidney function, Pacemaker syndrome, Inability to interrogate or program the LP due to programmer or LP malfunction, Intermittent or complete loss of pacing and/or sensing due to dislodgement or mechanical malfunction of the LP (non-battery related), Loss of capture or sensing due to embolization or fibrotic tissue response at the electrode, Increased capture threshold, Inappropriate sensor response, Interruption of desired LP function due to electrical interference, either electromyogenic or electromagnetic, Battery malfunction/ premature battery depletion, Device-related complications (Premature deployment, Device dislodgement/embolization of foreign material, Helix distortion), Death. As with any percutaneous catheterization procedure, potential complications include, but are not limited to: Vascular access complications; such as perforation, dissection, puncture, groin pain, Bleeding or hematoma, Thrombus formation, Thromboembolism, Air embolism, Local and systemic infection, Peripheral nerve damage. General surgery risks and complications from comorbidities; such as hypotension, dyspnea, respiratory failure, syncope, pneumonia, hypertension, cardiac failure, reaction to sedation, renal failure, anemia, and death.
Related articles
-
AVEIR DR System: 3 Things to Know After FDA Approval
With revolutionary tech and design, our FDA-approved system ushers in a new age for pacemakers.
-
Leadless Pacemaker Keeps the Beat? Bravo, Aveir! Bravo!
Aveir could treat slow heart rhythms — and can be retrieved later — all through minimally-invasive procedures.
-
Spend a minute with Matthew Fishler
Get to know Matthew Fishler, whose family history helped lead him to this: Developing the Aveir DR pacemaker.